Functional Medicine
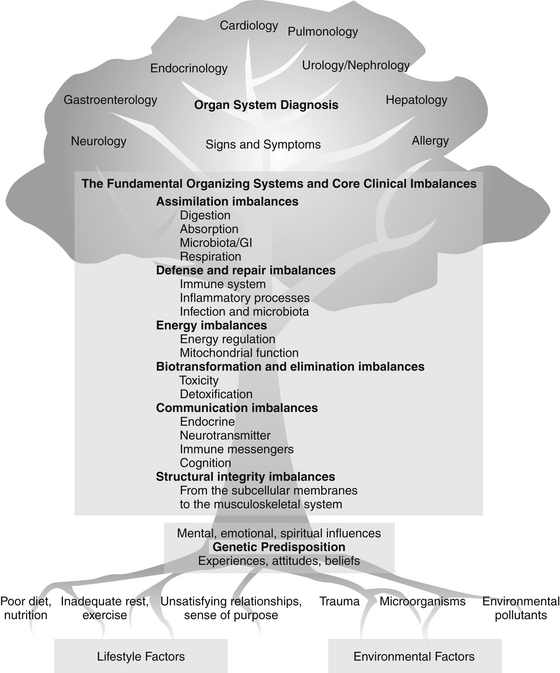
Functional medicine is an evolution in the practice of medicine that better addresses the healthcare needs of the 21st century. By shifting the traditional disease-centered focus of medical practice to a more patient-centered approach, functional medicine addresses the whole person, not just an isolated set of symptoms.
What Is Functional Medicine?
Functional medicine practitioners spend time with their patients, listening to their histories and looking at the interactions among genetic, environmental, and lifestyle factors that can influence long-term health and complex, chronic diseases. In this way, functional medicine supports the unique expression of health and vitality for everyone.
Why Do We Need Functional Medicine?
Our society is experiencing a tremendous increase in the number of people who suffer from complex, chronic diseases, such as diabetes, heart disease, gastrointestinal problems, cancer, mental illness, dementia, Alzheimer's autoimmune disorders like rheumatoid arthritis, and troublesome conditions like irritable bowel syndrome. Obesity and inflammation are other high-yield health problems that have a major contribution to chronic diseases.
The treatment that patients receive for these, and other chronic conditions is often inadequate. This is due, in part, to:
- Focus on acute care and symptomatic approach. The system of medicine practiced by most physicians is oriented toward acute care—the diagnosis and treatment of trauma or illness that is of short duration and in need of urgent care, such as appendicitis or a broken leg.
If a patient sees a doctor with high blood pressure, depression, joint pain, or any other chronic problems - the cure is only a “magic pill” - a drug. A quick fix!
The acute-care approach to medicine lacks the proper methods and tools to prevent and treat complex, chronic diseases.
- The gap between research and practice. The way many doctors practice isn’t up to date with new research. The gap between emerging research in the basic sciences and its use in medical practice is enormous—a few decades or more—particularly in the area of complex, chronic illness.
- Shortfalls in training. Medical providers are not adequately trained and do not spend appropriate time with patients to assess the underlying causes of complex, chronic diseases and to apply strategies such as nutrition, diet, and exercise to both treat and prevent these illnesses in their patients.
How Is Functional Medicine Different?
Functional medicine involves understanding the origins, prevention, and treatment of complex, chronic diseases. Hallmarks of a functional medicine approach include:
- Patient-centered care. The focus of functional medicine is on patient-centered care, promoting health as a positive vitality, beyond just the absence of disease.
- An integrative, science-based healthcare approach. Functional medicine practitioners look “upstream” to consider the complex web of interactions in the patient’s history, physiology, and lifestyle that can lead to illness. The unique genetic makeup of each patient is considered, along with both internal (mind, body, and spirit) and external (physical and social environment) factors that affect total functioning.
- A combination of best medical practices. Functional medicine integrates traditional Western medical practices with what are sometimes considered “alternative” or “integrative” medicine, creating a focus on prevention through nutrition, diet, and exercise; use of the latest laboratory testing and other diagnostic techniques; and prescribed combinations of botanical medicines, supplements, therapeutic diets, detoxification programs, or stress-management techniques.
